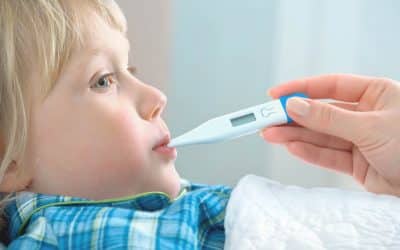
Baby acne only happens in your baby’s first few months of life
Neonatal Acne
Baby acne is a common, temporary skin condition that usually develops on a baby’s face. It looks like tiny red or white bumps or pimples. It occurs in about 20 percent of newborns.
Baby acne only happens in your baby’s first few months of life. In almost all cases, the acne resolves on its own without treatment.
What causes baby acne?
It’s unclear why baby acne develops, though many researchers and doctors think it is caused by maternal hormones.
Stork Bites
What Is A Stork Bite?
A stork bite, also known as a salmon patch or angel kisses, is a light pink- to red-colored flat birthmark that appears in 30% of newborn babies. The medical term is nevus simplex a and they are caused by irregular blood vessels underneath the skin. It may become more prominent when a child cries or has fever. Stork bites are usually found on the head, neck or face. The most common places are on the forehead, eyelids, nose, upper lip and back of the neck.
There is no specific testing that needs to be completed as a physician can determine whether your child has stork bite just by looking at it.
Mongolian Spots
Mongolian spots are very common birthmarks of dark-skinned babies. They are flat, brown/blueish in color and often look like a bruise. They are caused by pigment that didn’t come to the top layer when baby’s skin was being formed.
Erythema Toxicum
Erythema toxicum neonatorum is a common rash in neonates. It appears in up to half of newborns and starts within 3 days of birth. It looks like blotches of red, almost like hives. It usually fades within a week of birth and requires no treatment.
Milia
Milia are small white bumps that appear on the skin. They’re usually grouped together on the nose, cheeks, and chin, though they may appear elsewhere. They develop when skin flakes or keratin builds up and gets trapped under the surface.
Jaundice
Jaundice is a yellow pigment of the skin and the whites of the eyes. It is caused by excessive bilirubin, a product of the breakdown of red blood cells.
We normally notice jaundice in babies first in the whites of babies’ eyes. As the bilirubin level rises, we see the yellow moving down the body from the head to the toes.
Usually, jaundice appears within the first 24 hours of life, peaking at 3 to 5 days. Then it decreases over the next two weeks.
More than 50% of newborns develop jaundice in the newborn period, and only about 2% will have dangerously high levels. If bilirubin is too high it can be toxic to the brain.
The Canadian Pediatric Society and the American Academy of Pediatrics recommend that all babies be assessed within the first three days of life with a blood test or a transcutaneous measurement of the bilirubin level.
Your healthcare practitioner will then decide if the bilirubin level is too high and which treatment is necessary.
If your newborn has developed jaundice in the first 24 hours of life, is not feeding well, is not peeing or stooling enough, has fever or lethargy, the baby should be seen by a physician immediately. Most babies develop uncomplicated jaundice due to relative dehydration after birth. This is called breastfeeding jaundice. As mom’s milk comes in, baby usually gets more milk and jaundice fades.
Treatment
Most jaundice babies do not require any treatment. Typically jaundice will self-resolve if the baby is feeding well, and voiding and stooling adequately.
If the bilirubin level is excessive, some babies will require special lights called phototherapy lights to decrease the bilirubin level.
A small number of children will require a blood transfusion if the level is very high or not responding to phototherapy. Adequate hydration at this point with breastfeeding, formula feeding, or intravenous fluids is important.
Rest assured that if jaundice is detected and treated early, the vast majority of babies will thrive and develop normally.