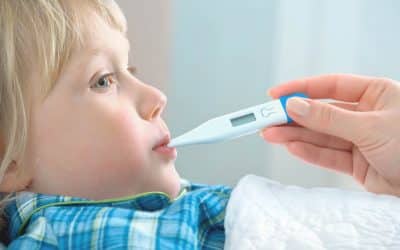
What is Child Asthma and What to Do?
Reactive Airway Disease (RAD)
RAD occurs when your bronchial tubes overreact and swell, causing breathing problems. Reactive airway disease is often diagnosed in young children showing signs of asthma but can’t be tested for lung function because they’re too small to undergo the procedure.
Asthma in Children
When parents hear they have a child with asthma or reactive airway disease, they are often fearful that their child will have a serious, life-threatening, life-long illness that may lead to frequent hospitalizations and long-term medication use.
Most cases of childhood asthma, or what we call ‘reactive airway disease,’ are otherwise healthy children with recurrent coughing or wheezing episodes.
This recurrent cough or wheeze is commonly triggered by a simple viral infection, which leads to an inflammatory response in the small airways. Many children will have issues with cough and wheeze when they are young and later outgrow it.
Childhood asthma is usually diagnosed clinically based on a child having recurrent episodes of wheezing or coughing.
Ask a Health Care Provider
Asthma in children rarely requires specialized testing called a methacholine challenge, which your primary care can order after kids eight years of age.
Before age 8, reactive airway disease is diagnosed clinically through the history of recurrent cough and wheeze, especially at night and in a viral illness setting.
Parents should be aware that a methacholine challenge is sometimes necessary after age 8 to diagnose reactive airway disease. This test can help determine if your child has asthma flare-ups or allergies and will show how strong their immune system response reacts to an allergen such as pollen.
Other health treatment options might be allergy medications or other asthma medicines.
What are the Symptoms of Reactive Airway Disease?
Symptoms of reactive airways disease:
- Wheezing
- Shortness of breath
- Chest tightness
- Coughing
- Mucous or sputum production or vomiting mucous
How do we Treat Reactive Airway Disease?
When a child has a cough that persists, or difficulty breathing, some specialists will prescribe puffers to help. Puffers can open up the airways to allow the child to breathe more easily, and they will help clear the mucus and inflammation that leads to cough and wheeze.
The most common puffers (asthma medications) we use in Canada are Salbutamol (Ventolin) and Fluticasone (Flovent). In other countries, different inhaled steroids may be used.
Asthma Attack
During an asthma attack, the airways are flooded with mucus and contract in such a way that they become blocked. The result is shortness of breath for you or your loved one who suffers from this condition.
The wheezing sound can be alarming during these attacks as it signals to those around us how much trouble we’re having breathing! During most severe cases, oxygen may need to be administered through nasal prongs until help arrives.
How do These Puffers Work?
Salbutamol (‘the blue one’)
Salbutamol is a bronchodilator. It opens up tight airways. Salbutamol works within 10-20 minutes and works for a few hours.
It is a rescue medication and is used when the child coughs or has difficulty breathing, up to every 4 hours as needed. Children will often need it before bed, when cough can be worse, during exercise, or at times of illness.
Fluticasone (‘the orange one’)
Fluticasone is an inhaled steroid and decreases mucus and inflammation in the small airways over days to weeks. It is prescribed to use morning and night. The medicine works to keep the lungs clear of inflammation.
Your child’s doctor might prescribe Salbutamol as needed for coughing or difficulty breathing. However, if your child needs to use the puffer every day, their asthma and cough are not adequately controlled.
Most children can take Fluticasone intermittently for a few weeks at a time when their asthma or cough is flaring up.
For virus-induced asthma or cough induced by a cold, I start Fluticasone at the beginning of the cold till a week or two after the cough resolves. This may keep it under better control and reduce visits to the emergency room.
Always use a spacer
(like Aerochamber):
The medicine doesn’t go to the lungs properly without a spacer device. These are plastic devices that space the medication from the mouth to allow the treatment to get into the lungs to do its work where it is needed.
Without one, most medicine goes to the back of the throat and not to the lungs where it is required.

FAQ’S
Is asthma in children hereditary?
Asthma is about 50% genetic, and this volume of research has encouraged the importance of family history.
Is covid 19 a type of asthma?
COVID-19 can cause shortness of breath and respiratory failure in people with severe diseases. However, it is not a type of child’s asthma.
Do I need to have an asthma action plan?
You should create an Asthma Action Plan to help you prevent and control your asthma attacks. Then, speak with a healthcare provider about developing options that suits your asthma symptoms because everyone is different!